Jawbone loss often goes unnoticed in many people – often painless, but with serious consequences. This condition not only jeopardizes the stability of the teeth but can also impair overall oral health in the long term. But what exactly causes jawbone loss, how can it be detected in time, and what can be done about it? This article is aimed at anyone who might be affected by jawbone loss due to periodontitis, tooth loss, or other causes and wants to learn more about the causes, the signs of recognition, and the treatment options for rebuilding or preserving bone mass.
In this article, you will read about the following: 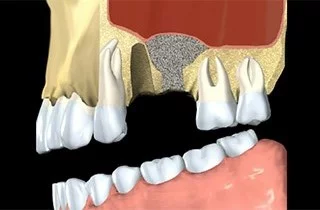
- What are the symptoms of dental bone loss?
- What are the causes of dental bone loss?
- Can teeth with bone loss be saved?
- Can you increase bone density after 30?
- Can you reverse dental bone loss?
What is dental bone loss?
Jawbone loss is in some ways similar to osteoporosis, as both involve the loss of bone mass, but they occur for different reasons and with different mechanisms of action. This condition causes a reduction in bone mass. Systemic bone loss is influenced by multiple factors, including hormonal changes, nutritional deficiencies, genetics, and physical activity levels. In contrast to general bone loss, other causes are responsible for bone loss in the jaw (also called jawbone loss).
What are the symptoms of dental bone loss?
In general, jawbone loss is very inconspicuous because it progresses painlessly. However, in the end, the entire jaw becomes less resilient. In an advanced state, you may notice the following symptoms: 
- gums bleeding when brushing teeth,
- red, swollen, and/or sensitive gums,
- bad breath,
- loose teeth,
- changes in how the teeth fit together.
What are the causes of dental bone loss?
Jawbone loss most often occurs as a result of periodontal disease or after the loss of several teeth that have not been replaced. Periodontitis is a gum disease. Poor oral hygiene can contribute to the development of jawbone loss, especially when combined with factors like genetic predisposition or advanced age. oral hygiene If this inflammation is not treated in time, it develops further into periodontitis, which ultimately leads to the breakdown of the jawbone.
Can teeth with bone loss be saved?
In many cases, yes – especially if the condition is diagnosed early. However, the main goal is usually to stabilise the tooth and stop further deterioration rather than to rebuild all lost bone. Whether a tooth can be preserved depends on how much supporting structure remains and how advanced the underlying periodontal damage is.
Early and targeted treatment can help maintain function and prolong the life of the natural tooth. Here’s how: Periodontal (gum) disease treatment: A deep cleaning procedure removes plaque and tartar from below the gum line, reducing infection and inflammation. In certain cases, topical or oral antibiotics may be prescribed. Some dentists also use laser-assisted therapy to support bacterial reduction and tissue healing. Gum grafts for receding gums: When gum recession exposes roots and weakens support, grafting procedures can improve soft tissue stability and protect the remaining bone structure. Splinting Loose Teeth: If teeth have become mobile but still retain sufficient support, splinting can help stabilise them, reduce discomfort during chewing, and limit further mechanical stress.
Saving a tooth with bone loss is often possible, but it requires realistic expectations and consistent follow-up care.
Can you increase bone density after 30?
Yes, you can increase bone density after the age of 30, but it becomes increasingly difficult as bone mass naturally declines. Although the potential for bone building is highest before the age of 30, it is still possible to increase or maintain bone density into adulthood with consistent attention and a healthy lifestyle. Eat for strong bones: Consume foods rich in calcium and vitamins D and K, and Magnesium. Weight-bearing and strengthening exercises: Activities such as walking, jogging, dancing, and resistance training stimulate bone turnover. Lifestyle changes: Quit smoking and limit alcohol, maintain a healthy weight. Regular checkups and bone density tests: A DEXA scan can assess bone health and help track progress.
Can you reverse dental bone loss?
Complete reversal of advanced dental bone loss is uncommon. However, modern regenerative dentistry can rebuild bone volume in specific clinical situations, particularly when preparing for implants or restoring structural support.
Here are some approaches:
Bone grafting: It can help reconstruct deficient areas if bone loss has occurred due to missing teeth or advanced periodontal disease. Natural or synthetic graft material is placed into the affected site to stimulate new bone formation. Guided bone regeneration (GBR): This technique uses barrier membranes to create a protected space where bone cells can regenerate without interference from surrounding soft tissue. Dental Implants and Osseointegration: When a dental implant is placed into regenerated bone, the process of osseointegration helps maintain bone stimulation and long-term structural stability.
Platelet-Rich Plasma (PRP) Therapy: PRP may support healing in certain cases, although scientific evidence regarding long-term bone regeneration outcomes remains mixed. Growth factors derived from the patient’s own blood can support healing and tissue regeneration. Medications and Supplements: While certain medications such as bisphosphonates are primarily used in osteoporosis management, adequate calcium and vitamin D intake contribute to overall bone metabolism. Preventing further bone loss: Long-term success depends on controlling inflammation, replacing missing teeth to restore mechanical stimulation, and maintaining consistent oral hygiene. Read more about stopping jawbone loss and jawbone augmentation costs, After a bone augmentation
Frequently Asked Questions about dental bone loss
- Does dental bone loss affect facial appearance over time?
Yes. Progressive bone loss can reduce jaw support, leading to subtle facial collapse, thinner lips, and deeper nasolabial folds. In advanced cases, the lower face may appear shorter due to reduced vertical dimension. - How quickly can dental bone loss progress after a tooth extraction?
Bone resorption can begin within weeks after extraction. The most significant volume reduction usually occurs during the first 3–6 months, especially if no implant or bone preservation procedure is performed. - Can dental bone loss occur even with good oral hygiene?
Yes. While poor hygiene is a major risk factor, genetic predisposition, systemic conditions such as diabetes, smoking, and long-term inflammation can also contribute to bone loss despite careful brushing and flossing. - Is dental bone loss visible on regular dental X-rays?
In most cases, yes. Standard panoramic or periapical X-rays can reveal bone height reduction, while 3D CBCT imaging provides more detailed information about bone volume and density. - Does wearing dentures accelerate dental bone loss?
Traditional removable dentures do not stimulate the jawbone like natural teeth or implants. Over time, this lack of stimulation may contribute to continued bone resorption in edentulous areas. - Can orthodontic treatment help prevent dental bone loss?
When properly planned, orthodontics can improve bite distribution and reduce traumatic forces, indirectly protecting supporting bone structures. However, it cannot rebuild already lost bone. - Are smokers at higher risk for dental bone loss?
Yes. Smoking reduces blood supply to the gums, impairs healing, and increases susceptibility to periodontal disease, all of which significantly raise the risk of progressive bone destruction. - What is the long-term risk of untreated dental bone loss?
If left untreated, bone loss can lead to tooth mobility, tooth loss, bite collapse, and more complex restorative needs. Early diagnosis allows for more conservative and predictable treatment options.
Although severe bone loss is difficult to reverse completely, modern dental treatments can restore function and, in selected cases, partially rebuild lost bone structure.

